High Quality Ileostomy Surgery
Price :- From $ 5000
Ileostomy surgery at low cost and high quality is now within reach through HealthCare Travel Council Of India. Our nurses arrange all aspects of your treatment and will act as your patient advocate.
What is an ileostomy?
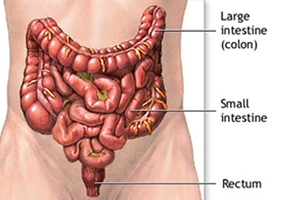
The ileum is the lower section of the small bowel. It connects to the large bowel. If a portion of the large bowel has to be removed due to bowel disease, ileostomy surgery is performed.
An ileostomy creates an opening in the ileum to allow waste elimination. An ileostomy can be either temporary or permanent. Medical conditions, which may cause the necessity for an ileostomy, are:
- Severe inflammatory bowel disease
- Bowel injuries
- Bowel obstruction
- Bowel cancer
- Bowel infections
Ileostomy surgery
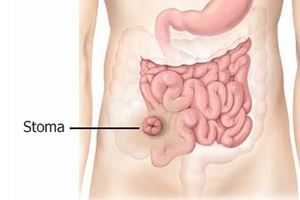
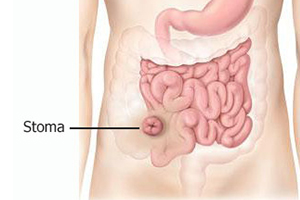
An ileostomy procedure is performed under general anesthetic. An opening in the side of your abdomen will be created by the surgeon. This is called a “stoma”. Usually the stoma is on your right lower abdomen. The surgeon will remove the portion of the bowel that is causing your medical condition. For a traditional ileostomy, a section of the ileum is then extracted through the opening and sutured to your abdominal skin. An adhesive plastic bag is placed on the abdomen over the stoma for waste evacuation.
With a traditional ileostomy, bowel contents continuously drain into the ileostomy bag. With a continent ileostomy, there is no waste bag. Instead, an internal pouch made from intestinal tissue is created and attached to the abdominal wall. Waste contents to do not continuously drain. In this case, the pouch is emptied with a narrow tube inserted into the pouch anywhere from 2 to 7 times daily. There are risks involved with ileostomy surgery.
These include general anesthetic risks, bleeding, infection, hernia, scarring, stenosis (narrowing) of the stoma, bowel obstruction and dehydration. Your doctor can give you complete information regarding all the risks surrounding ileostomy surgery.
Ileostomy preparation
Preparation for an ileostomy can begin up to two weeks prior to the surgery date.
Your doctor may request you stop taking anti-coagulant medications (aspirin, Advil, anti-inflammatories) at this time. If you have a cold or flu prior to your surgery date, you need to let your doctor know as soon as possible.
Surgery may have to be delayed if this is the case. You should drink lots of water and eat a high fiber diet. Closer to your surgery, you will likely be asked to start a clear fluids only diet. No fluids or foods will be permitted after midnight the evening before your surgery. You may be given antibiotics prior to surgery to remove bacteria from your colon. Additionally, you will be placed on a bowel-cleansing regime with laxatives or enemas a day or two before the procedure.
Your bowel must be empty and clean for surgery to prevent infection. You will be in the hospital 6 to 10 days after surgery.
If necessary, you should arrange, in advance, for:
- Child care
- Pet care
- A house sitter, if necessary
- Payment of your financial obligations
Ileostomy recovery
After surgery, you will be given a fluid diet until your bowel begins to function again.
Once this happens, solids will be gradually permitted.
This may be within two days or may take a little longer. Before discharge from hospital, you will be taught how to use a stoma pouch and care for your stoma.
It is important the area around the stoma be kept clean to reduce skin irritation. Stoma pouches are odor-resistant and invisible under your clothing.
Emptying the pouch when it is 1/3 full prevents bulging that may become apparent.
The number of times a pouch needs to be emptied daily varies widely.
After the first six months, you may find the necessity to empty the pouch decreases.
Pouches are replaced every 3 to 7 days. You should avoid strenuous exertions for the first three months after your surgery.
Normal everyday activities can resume 4 to 8 weeks post-surgery.
The average return to work after an ileostomy is 2 to 3 months. Using a stoma pouch may be difficult to adjust to in the beginning.
In time, you will be more at ease with the care and use of a stoma pouch.
This may take several weeks to months. Requiring ileostomy surgery and a stoma pouch can be psychologically distressing.
If you are experiencing anxieties, you should speak with your health professionals about coping strategies.
Contacting a support group may also be beneficial. Patients who undergo an ileostomy often have an improved quality of life.
They are freed from the symptoms of the medical condition that necessitated the ileostomy and are able to enjoy activities they may not have been able to participate in prior to surgery.
What is a colostomy?
Price :- From $ 5500
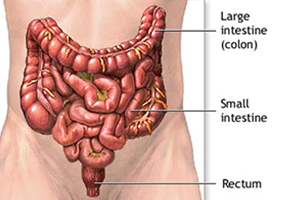
A colostomy is major surgery that creates an opening (known as a “stoma”) in the colon to permit waste to exit outside the body into a pouch attached to the abdomen. Generally, in a colostomy, part of or the entire colon is removed.
A colostomy may be permanent or temporary, depending on the medical condition that has necessitated the surgery. A temporary colostomy is to allow the colon to rest after surgery.
In time, the two sections of the colon will be reconnected and the bowels will work in the normal fashion.
A permanent colostomy is customarily performed when the rectum or most of the colon is removed.
- Colon cancer
- Diverticulitis
- Crohn’s Disease
- Colon obstruction
- Birth defects
There are different types of colostomies:
- Ascending: This is the least common type of colostomy. A stoma is made in the first section of colon, the ascending colon, on the right abdomen. The skin is easily irritated with this kind of stoma because the stool contains digestive enzymes and is mostly liquid.
- Transverse:Two separate stomas are created in this form of colostomy. These stomas can be located in the upper abdomen, middle or right side. One stoma is for the evacuation of stool waste and the other stoma is to allow mucus to drain. The stool is liquid to semi-formed. This is often a temporary colostomy
- Descending or Sigmoid: The stomas are located on the descending or sigmoid portion of the colon. The stomas are usually created on the left lower abdomen. Stool is semi-formed to fully formed. A descending or sigmoid colostomy is the most commonly performed permanent colostomy surgery. Approximately 42,000 to 65,000 ostomy surgeries are performed each year. Half of these surgeries are temporary.
Colostomy surgery
A colostomy is performed under general anesthetic. You will be unconscious and not feel any pain.
You may have a tube inserted through your nose into your stomach. This tube removes gas and prevents nausea and vomiting. It is possible a urinary catheter will also be used.
A colostomy can be carried out as open surgery or laparoscopically (several small surgical incisions are used to insert an instrument called a laparoscope which views and completes the operation).
Regardless of the method of surgery, the surgeon will remove the part or all of the colon that is diseased or malfunctioning. The healthy end of the colon will be brought to an abdominal opening made by incision and sewn to your abdominal skin.You may have drainage tubes in your incision.
After surgery, you go into the recovery room for monitoring until the anesthetic has worn off.
You will then be taken to your hospital room.
- Hernia
- Stomal tissue death
- Narrowing of the stoma opening
- The stoma retracts to inside your abdomen or even with the abdominal surface
- The stoma extends beyond the abdominal opening
- Pneumonia
- Infection
- Excessive bleeding
- Pulmonary embolism
There are risks connected to general anesthetic as well. Consultation with your doctor about all the risks of undergoing a colostomy is strongly recommended.
Colostomy recovery
You will be kept in hospital for up to one week. The first days after surgery, you will only be permitted fluids through an IV until your bowels begin functioning. The nurse will assist you to walk or stand as early as possible. Pain medication will be supplied.
Once your stoma starts to work, you will be allowed clear fluids with a steady progression to solid food.
You will be taught about colostomy care and supplies while in the hospital. After discharge from the hospital, you can expect a six-week recovery at home. Dietary counseling may be advised to help your bowel function. As well, psychological counseling may be appropriate. Many patients find it emotionally distressing to wear a colostomy pouch and feel it will interfere with many aspects of their life.
After a period of adjustment, most patients become accustomed to the colostomy and lead fulfilled lives.
Why is Colorectal Surgery needed?
Price :- From $ After Evaluation
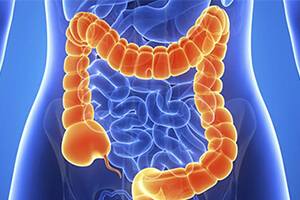
Colorectal surgery is mainly done to repair any kind of damage suffered by a patient’s anus, rectum or colon. This damage to these parts could be the result of a medical disorder, disease of the lower intestinal passageway, injury/obstruction as well as damaged blood vessels that require surgical procedure for repairing.
At times, abnormal tissue mass, or scar tissue can be seen developing within the rectum, which results in blocking the natural passing of bowels. There are also other common medical diseases, such as ulcerative colitis and diverticulitis that are known to cause damage to the rectum. Removing the obstruction or treating these parts with surgical procedures is known to be the ideal treatment method for restoring normal bowel movement and overall health in the patient.
What are the types of Colorectal Surgeries?
As mentioned earlier, colorectal surgery is an umbrella term including a number of surgical procedures that are useful for variety of medical disorders affecting anus, rectum or colon. This treatment is ideal for colorectal cancer, Cohn’s disease, ulcerative colitis, certain types of diverticulitis and other medical disorders that cause an obstruction in the lower intestine passage. Hemorrhoids, bowel incontinence, rectal prolapse and anal fissures may also require a person to have minor form of colorectal surgery for better treatment.
Most colorectal surgeries are aimed at repairing torn inner tissue, remove obstructions or to tighten the sphincter muscles. Certain colorectal specialist surgeons are also known to successfully treat pelvic floor disorders, such as perineal hernia and rectocele with colorectal surgery.
As mentioned earlier, colorectal surgery contains several different types of surgical procedures that are meant to treat a specific colorectal disorder. These are the common types of colorectal surgeries:
Resection – Resection involves cutting/removing the damaged/diseased portion of the lower intestine.
Anastomosis – Anastomosis involves re-attaching the resection ends of the lower part of the intestines together.
Tucks – Tucks are small surgical procedures that involve tightening the loosened/prolapsed sphincter muscles, as well as to repair anal fissures and to remove hemorrhoids.
Strictureplasty – Strictureplasty is an innovative colorectal surgical procedure that involves widening the intestine to make it shorter in length. This treatment is ideally used to treat extensive damage from Crohn’s disease.
Ostomy – These are a collective bunch of colorectal procedures that are basically aimed at creating an o
pening from the intestine to outside the body for passing bowel through an alternate route. A colostomy connects the large intestine to an opening in the abdomen (stoma) which passes bowels out of the body into an attached pouch. Ileostomy requires removing the anus, rectum and colon completely, and making the small intestine a stoma (opening in abdomen).
When is Colorectal Surgery needed?
Colorectal surgery is not always the first choice of treatment in mild cases of medical disorder affecting the colorectal region. However, the doctor/physician will decide whether you will need a colorectal surgery, after considering various factors, such as your age, health status, underlying medical disorders, etc as well as the extent of spread and damage by the disease.
As most often, there has to be significant changes made in your lifestyle after certain colorectal surgeries, the doctor/physician/surgeon will advise you on all the pre-surgical and post-surgical care which you will be required to take for best results.
Are there any risks associated with Colorectal Surgery?
As is seen in any major surgery, colorectal surgical procedures are also not completely devoid of certain surgical risks, such as:
- Infection
- Swelling
- Pain
- Hemorrhage
However, the surgeon will ensure every preventive measure is taken to avoid these risks from developing.
HealthCare Travel Council Of India is the leading medical tourism healthcare provider. HealthCare Travel Council Of India maintains a vast network of global-standard hospitals in major destinations across the world, including India, US, UK and Dubai among others for the best treatment to patients. HealthCare Travel Council Of India offers effective, fast and affordable colorectal surgeries to patients from all over the world.
What is Prostate Cancer?
Price :- From $ 4500
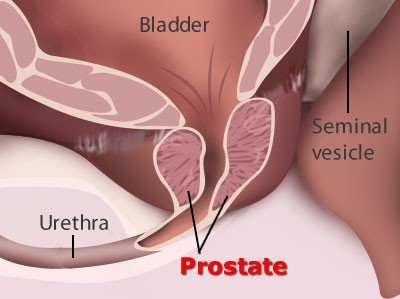
Prostate cancer is a common cancer seen in men. Prostate cancer affects the prostate gland.
This is a small gland which is located in the lower back. The prostate gland is responsible for
producing the seminal fluid which is vital to nourish and transport the sperm.
Usually, the prostate cancer may develop in the prostate gland slowly without spreading the
infection outside the gland. This is often a benign prostate cancer that can be treated quite
easily comparatively. However, other types of prostate cancers are seen to be more aggressive
and affect the prostate gland and then start to spread to the surrounding healthy tissues and
organs as well.
Prostate cancer can be treated more effectively when it is detected in its earlier stages.
What are the signs and symptoms seen in Prostate Cancer?
Prostate cancer might not exhibit any signs and symptoms in its early stages. However, as the
cancer develops there might be visible signs and symptoms, such as:
Decreased urine force
Trouble urinating
Blood in semen
Pelvic pain or discomfort
Bone ache
Erectile dysfunction
It is highly advised to consult an experienced oncologist in case any of these signs and
symptoms is noticed.
What causes Prostate Cancer?
Although the exact cause for the initiation of prostate cancer is not yet known the doctors
identify the mutation of the abnormal cell’s DNA to be the result in the uncontrolled growth of
the affected cells and form the cancerous tissue (tumor) in the prostate. This abnormal mass of
cells (tumor) can also spread (metastasize) to the surrounding healthy tissues and cause the
cells to mutate.
How is Prostate Cancer diagnosed?
Doctors advise men over 50 to have regular annual or bi-annual screenings for prostate cancer.
As early detection can help treat prostate cancer effectively regular screening will help identify
any possible cancer risks and eliminate them beforehand.
The screening tests for prostate cancer may include:
DRE (Digital rectal exam) – This involves a physical examination of the patient’s rectum by the
doctor using a gloved and lubricated finger. This helps the doctor identify any abnormalities in
the size and shape of the gland.
PSA (Prostate specific antigen) – This involves taking a blood sample from the arm to analyze
for PSA, which is naturally produced by the prostate gland. An abnormal level of PSA in the
blood will indicate towards an abnormality in the prostate gland.
To diagnose prostate gland, the doctor will perform the following diagnostic tests:
Ultrasound – This test allows the doctor to get a clear image of the inside of the rectum and the
prostate gland using a trans-rectal ultrasound probe.
Prostate biopsy – This involves removing a sample of the suspected cancer tissue using
minimally invasive methods. This tissue sample is then analyzed in detail in a pathology
laboratory to determine the presence of cancerous cells.
The biopsy will also help to determine the staging (severity) of the prostate cancer. This helps
to determine the best-suited treatment method for the particular case.
Staging is also done by a series of other diagnostic tests, including:
- Ultrasound
- Bone scan
- CT(computerized tomography) scan
- MRI (magnetic resonance imaging) scan
- PET (positron emission tomography) test
How is Prostate Cancer treated?
The treatment of prostate cancer mainly depends on the rate of growth (malignancy) of the
cancer as well as the extent of its spread (metastasizing). The overall health status will also help
decide the best-suited treatment for the particular case.
Although, in the early stages of prostate cancer as well as many cases of smaller prostate
cancer, the cancer is mostly benign and does not pose a threat right away. At times, the cancer
recedes and disappears on its own. Active surveillance may be advised in such cases, which will
involve regular blood tests and rectal exams.
Radiation therapy
Radiation therapy (radiotherapy) uses powerful beams of particles to target and destroy the
cancerous cells effectively. This treatment is administered in two different ways:
External beam radiation – This involves using a large machine to direct the particle rays on to
the body from outside. These are targeted on the prostate cancer and help destroy the cells
with the heat generated.
Brachytherapy – This is an internal prostate cancer radiotherapy treatment technique. It
involves inserting a small (rice-sized) radioactive seed in the prostate tissue using minimally
invasive methods. This seed is programmed to give out precise dosage of radiation right into
the prostate cancer tissue.
Hormone therapy
This therapy involves administering special drugs that are used to control the production of
testosterone in the body. Lack of testosterone is known to affect the nutritional supply of the
prostate cancer cells and eventually destroy them.
Surgery
Surgical removal of prostate cancer involves radical prostatectomy. In this, the surgeon will use
varying techniques and methods to remove the cancer-affected prostate gland in a safe
manner. The surgeon may use advanced robotic-assisted surgery in order to reduce recovery
time and get more effective results.
Cryotherapy
This treatment involves freezing the cancerous prostate cancer tissue using super-cooled
substances. Thin long needles are used to inject the prostate cancer with the freezing agent. A
second injection delivers a heating agent which allows the frozen cells to thaw. This process
helps kill off the cancer cells effectively.
Chemotherapy
This involves administering specialized drugs to fight the cancer cells in the prostate gland. The
drugs may be administered using injection, IVs or as oral dosage.
Biological therapy
Also known as immunotherapy, this prostate cancer treatment method involves administering
special medicines that strengthen the body’s immune system and help fight the cancer cells
naturally.
HealthCare Travel Council Of India has been involved in providing all-round assistance to patients for
travelling abroad to some of the most popular international destinations and get highly-
effective and advanced prostate cancer treatments. These prostate cancer treatments are
delivered at the hands of the most experienced cancer specialists at the most affordable cost to
the patient.
What is Melanoma?
Price :- From $ 3000
Melanoma is a serious form of skin cancer and is quite common today. Melanoma develops in the melanocytes, which are cells that produce melanin. Melanin is the natural pigment that gives tone and complexion to the skin.
Melanoma can develop in the eyes and also rarely in the internal organs, such as the intestines.
What are the signs and symptoms of Melanoma?
Melanoma develops almost anywhere on the body but is mostly seen affecting areas that are more exposed to the sun, including face, arms, legs and back.
Melanoma also develops in covered areas of the body, including the soles of feet, palms and even the fingernail beds. These types of melanomas are mostly seen in people with a darker skin complexion.
These are the initial signs of melanoma:
- Change is appearance of existing mole
- Occurrence of new abnormal skin growth
Melanoma does not always develop in the form of a mole but it is also seen in normal-seeming skin as well.
Identifying melanomas is comparatively easy if you know what to look for. These are some of the factors that help identify the cancerous nature of abnormal skin formations, such as moles.
Although most moles tend to be benign and superficial, similar moles are known to later develop into serious melanomas.
Identifying melanoma
Check for the following points in the mole to check if it is a melanoma:
- Asymmetrical shape
- Irregular border
- Color change
- Large diameter
- Evolution/developmental changes
Malignant (cancerous) moles can be of various appearances. At times, most of the above-mentioned signs can be seen in melanoma moles or they may show only one of the aspects of change in appearance.
Areas where melanomas develop are mostly on sun-exposed regions of skin, however, there are other places, such as between toes, on soles, palms, scalp, etc where melanoma can develop too. These are also called as hidden melanomas.
These are the regions where hidden melanomas are generally seen:
- Under the nails
- In the mouth
- Digestive tract
- Urinary tract
- Vagina
- Eye
It is advisable to consult a doctor when any of the signs and symptoms of melanoma are seen for best and most effective treatment.
What are the causes of Melanoma?
Melanomas are known to start when the melanocytes (melanin-producing cells) start to malfunction. Damage to the cellular DNA is known to result in abnormal growth of skin cells from it.
The exact cause of damage to the cellular DNA of melanocytes is not yet known the overexposure to sun or UV radiation is known to increase the risk of developing melanoma significantly.
How is Melanoma diagnosed?
There are several ways to determine the presence of melanoma as well as to determine the stage (level of development) of the melanoma.
These are the diagnostic tests that help determine the presence of melanoma in a person:
Physical examination – This involves the doctor inspecting every part of the skin to check for visible signs of melanoma.
Biopsy – This is a minimally invasive surgical technique to remove a sample of the suspected melanoma tissue. In this, the surgeon will remove the complete (or part of) the suspected mole and send it for detailed analysis at the pathology laboratory.
There are several different techniques used in biopsy for a melanoma, including:
- Punch biopsy – This requires using a circular-bladed small surgical tool, very similar to a conventional punching machine, which helps to make a perfectly round incision around the mole. This helps to remove the suspected mole as well as the surrounding skin tissue.
- Excision biopsy – The surgeon uses conventional surgery methods to remove the entire suspicious mole along with a margin of skin from the surrounding.
- Incision biopsy – The surgeon will use more precision to remove only the abnormal looking part of the suspected mole.
Staging of Melanoma
Staging of melanoma helps to determine the extent of the cancer. The doctor will check the following to determine the stage of the melanoma:
- Thickness – The melanoma’s thickness is judged using a powerful microscope and using a micrometer to measure it.
- Spread – The extent of spread of melanoma to nearby lymph nodes is checked.
How is Melanoma treated?
Melanoma is treated using several different methods. The exact type of melanoma treatment mainly depends on the size and the extent (stage) of the cancer. The doctor will also consider the patient’s age and overall health in order to choose the best treatment method.
The treatment for early-stage melanoma is done with surgery. The surgeon will peel off very thin payers of the affected skin for biopsy or remove the entire melanoma along with a margin from the surrounding healthy tissue.
For metastatic melanoma, that has spread to other organs there are several different treatment techniques, such as:
Surgery for lymph node removal
In case the melanoma is seen to affect the nearby lymph node then the surgeon will choose the remove the affected lymph nodes. This is often combined with another pre-surgical or post-surgical treatment.
Chemotherapy
This uses specially designed drugs to destroy the cancer cells. Chemotherapy drugs are administered using oral or intravenous, as well as a combination of both, techniques.
This is usually given in an isolated limb perfusion technique when the melanoma is seen affecting a specific part of the body, such as the arm or leg. This helps restrict the effects of the drugs to the affected area only.
Radiotherapy
Radiation therapy uses high-energy beams of radiation (x-rays, etc) particles to target the cancerous cells precisely. Radiotherapy is often used in combination with surgical cancer treatment to shrink the size of the cancerous tissue which can be then easily removed with surgery.
Biological therapy
This is an immune-boosting technique to fight cancer cells naturally. Specially designed medicinal drugs are used in this to strengthen the immune system and fight the melanoma.
Targeted therapy
This melanoma treatment therapy uses special medicinal drugs that are designed to target the weakness of the cancer cells. Advanced melanoma can be effectively treated using expert targeted therapy.
Why choose HealthCare Travel Council Of India for Melanoma treatment?
HealthCare Travel Council Of India is the renowned medical tourism company in the world. Wide State is associated from a long time with numerous advanced oncology specialty hospitals. This forms a global network of the best and most reliable cancer-specialty healthcare centres for melanoma treatment through HealthCare Travel Council Of India. HealthCare Travel Council Of India ensures that each patient gets the best and melanoma treatment abroad at the hands of the most expert cancer specialists.
What is Deep Brain Stimulation?
Price :- From $ 15000
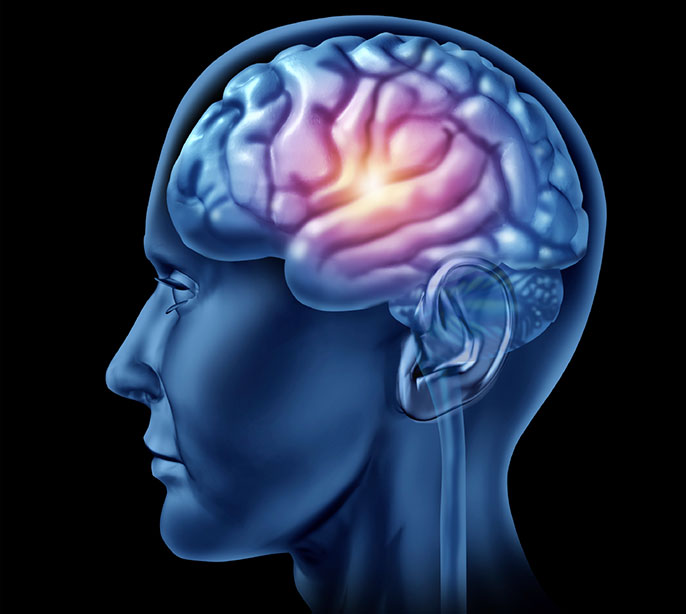
Deep brain stimulation is an innovative neurological treatment technique. It involves implanting tiny electrodes in specific areas of the brain to transmit electrical impulses to regulate abnormal neural impulses. Certain mental and physical disorders can be traced to bnormal neural impulse activity and chemical imbalance.
How is Deep Brain Stimulation treatment performed?
Although the surgical approach may vary from surgeon to surgeon the end goal of the surgery is to fix a device in the chest which is connected through small wires to four electrodes in the brain.
A device similar to a pace-maker is used to control the intensity and frequency of the artificial electrical impulse in deep brain stimulation treatment method. This device is placed mostly under the collarbone, with wires tiny wires running under the skin to connect to the electrodes in the brain.
The surgeon will choose the trouble spots in the brain where abnormal neural activity is resulting in the symptoms or disorder. This is a local anaesthesia procedure where the patient is kept awake during the surgery to gauge the activeness of the brain functions.
Patients are usually required to rest in the hospital for at least 3 days after the deep brain stimulation device implanting surgery.
What is Deep Brain Stimulation useful for?
Deep brain stimulation technique is an ultra-modern neurological treatment method for various diseases and disorders, such as:
- Parkinson’s disease
- Slight tremors
- Epilepsy
- Dystonia
- Chronic pain
- Tourette syndrome
- OCD (Obsessive Compulsive Disorder)
The deep brain stimulation technique also shows effective results in treatment of addiction, dementia, depression and rehabilitation after recovery from a stroke.
Deep brain stimulation treatment is mostly advised when a person suffering from movement disorders (including dystonia, OCD, Parkinson’s disease, etc) does not find relief after treatment with medications.
Are there any risks associated with Deep Brain Stimulation treatment?
Although deep brain stimulation is a minimally invasive surgery there are still certain risks in rare cases, as in seen in any form of surgical treatment.
Risks from surgery – As deep brain stimulation involves implanting electrodes the surgeon will have to drill small holes into the skull. The device with the regulator and power will also have to be surgically implanted in the upper chest.
Surgical risks
- Stroke
- Bleeding
- Infection
- Nausea
- Breathing problems
- Seizures
- Heart problems
Side effects of stimulation
Once the device and electrodes are implanted the surgeon will wait for several weeks before starting the device. This step requires searching for the ideal setting for the particular patient this may initially produce certain side effects, such as:
- Muscle tightness in arm or face
- Numb/tingling sensation
- Balance problems/vertigo
- Speech issues
- Unpredicted mood swings
- Light headedness
These are seen in rare cases and mostly disappear as the ideal electrical stimulation frequency is discovered.
Why choose HealthCare Travel Council Of India for Deep Brain Stimulation treatment?
HealthCare Travel Council Of India is a leading global medical tourism service provider. Wide State is renowned for providing efficient services with overall assistance to patients who wish to travel abroad for a wide variety of medical treatments. HealthCare Travel Council Of India is associated with the largest network of global-class neurological healthcare institutes all around the world. These are all high-tech neurology surgery specialty hospitals located at popular international destinations. Wide State offers complete assistance to patients to travel abroad to the destination of their choice and get the best and most effective deep brain stimulation treatment at the most cost-efficient price.
What is T-Cell Leukemia?
Price :- From $ 7000
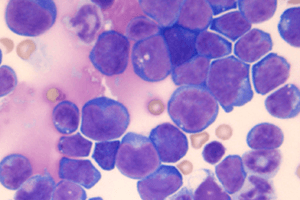
T-cell leukemia is also called as ‘chronic t-cell lymphocytic leukemia’. It is a type of CLL (or Chronic Lymphocytic Leukemia) which affects the white blood cells (WBC) that are responsible for strengthening the immune system to fight against infection.
What are the types of T-Cell Leukemia?
These are the various four type of t-cell leukemia:
LGLL (Large Granular Lymphocytic Leukemia) – This is a slow-growing type of t-cell leukemia which is found to be more prominent in women, than in men. The exact cause for this blood cancer is not known.
T-PLL (T-cell Prolymphocytic Leukemia) – This is a dangerous form of t-cell leukemia and is found to affect and spread comparatively faster. This t-cell leukemia type affects mainly adults and is more common in senior males than females. This mostly affects the skin quality.
ATLL (Adult T-cell Leukemia/Lymphoma) – This T-cell leukemia is further sub-divided as adult, acute, chronic and smoldering T-cell lymphoma. This is a cancer of the lymphatic system and is identified by their specific features.
Sezary Syndrome – This is a form of mycosis fungoides which mainly affects the skin. This is normally a slow-growing type of T-cell leukemia and is usually diagnosed by the increasing numbers of lymphoma cells in the blood, which is often accompanied by the reddening of the skin.
What are the signs and symptoms of T-cell Leukemia?
At times, a case of T-cell leukemia might not show any signs otherwise there are several commonly seen signs and symptoms that can be used to identify T-cell leukemia, such as:
- Frequent infections
- Unexplained chills/fever
- Bleeding easily
- Easy bruising
- Constant fatigue
- Constant pain in the left abdominal region
- Swollen lymph nodes
- Skin lesions
- Rash
- Frequent urination
- Constipation
- Itching of skin
- Feeling full with comparatively less diet
How is T-cell Leukemia diagnosed?
Initially the doctor will perform a complete physical examination and check for the signs and symptoms as well as the medical history.
These are the other diagnostic tests that help the doctor determine the type of leukemia as well as the ideal treatment for it:
- Blood tests – Extensive range of blood testing is available, such as CBC (complete blood count) in which the level and condition of the various types of blood cells can be estimated.
- Biopsy/Bone Marrow Aspiration – Both these procedure are performed simultaneously to examine the bone marrow in detail. Bone marrow aspiration involves removing the liquid part of the bone marrow using a thin long needle. A biopsy involves removing a small part of the bone for detailed analysis at the pathology laboratory.
- Skin biopsy – This involves surgically removing a small portion of the affected skin to be examined in detail in a pathology laboratory.
- CT (computerized tomography) scan – This advanced imaging diagnostic testing helps the surgeon get a 3D image of the affected body part without the need for intrusive methods.
How is T-cell Leukemia treated?
There are various ways to effectively treat the different types of T-cell leukemia.
These are the various types of treatments for T-cell leukemia:
Chemotherapy
This involves using a combination of special medicinal drugs. These are designed to target the cancerous cells involved. The chemotherapy treatment can be administered as oral medications, injections or IV tubes.
Chemotherapy is a gradual process and the doctor will administer it according to a set regimen.
Immunotherapy
This is also known as biologic therapy. It is aimed to boost the body’s natural immune system in order to fight the cancerous leukemia cells in the blood.
This uses a combination of natural and artificial substances to increase the strength of the patient’s own immune system to effectively destroy cancerous leukemia cells.
Targeted therapy
This is an accurate treatment which targets the cancer’s genes and supportive environment that helps it to grow.
This therapy blocks the supply of protein and nutrients to the cancerous cells and help to destroy it completely.
Radiotherapy
This treatment method for T-cell leukemia uses high-energy beams of x-rays (or other particles) to target and destroy leukemia cells in the blood.
This treatment is commonly performed as an external-beam radiation therapy in which the radiation is emitted from a huge machine in which the body is placed. Another form of radiotherapy is internal radiation therapy (brachytherapy) which requires inserting a small radioactive device into the body and emit radiation on the cancerous cells from a closer range for maximum effectiveness.
Surgery
Surgical treatment of T-cell leukemia mainly involves a splenectomy in which the surgeon will remove the white blood cell-producing spleen. This is to stop the growth of cancerous cells which are affected after being continuously produced by the spleen.
Why choose HealthCare Travel Council Of India for T-cell Leukemia treatment?
HealthCare Travel Council Of India is the most reliable and efficient medical tourism service provider today. The company is strongly associated with a large number of global-class oncology specialty hospitals all across the world. This allows HealthCare Travel Council Of India to arrange for the best and most convenient T-cell leukemia treatments for each patient at popular destinations abroad. HealthCare Travel Council Of India ensures easy, efficient and cost-effective T-cell leukemia treatment for all.
What is Breast Cancer?
Price :- From $ 3500

Breast cancer is the cancerous tissue that develops in a woman’s breasts. Breast cancer causes the breast tissue cells to become cancerous and multiply at an abnormally fast rate. This mostly results in the formation of a tumour (hard cancerous mass) in the breast which can be distinctly felt.
What are the signs and symptoms of Breast Cancer?
There are several common and some distinct signs that are seen when a breast cancer develops.
The signs and symptoms of breast cancer include:
- Lump in breast
- Change in size/shape/appearance of breast
- Change/new dimple on breast skin
- Recently inverted nipple
- Peeling/flaking of skin around nipple (areola)
- Redness over breast skin
The cause for the development of breast cancer is yet unknown however, when the cancer affects the breast it results in abnormal development of breast tissue cells. The cancer-affected cells in the breast begin to multiply faster and uncontrolled which then begin to form lumps (tumorous growths). Breast cancer is also known to spread (metastasize) to the other surrounding tissue and organs, including the lymph nodes.
Breast cancer is mostly seen beginning in the tissue cells of the milk-producing ducts (also known as invasive ductal carcinoma) or it may begin in the lobules (invasive lobular carcinoma) as well as any other part of the breast.
How is Breast Cancer diagnosed?
Breast cancer is treated successfully when it is diagnosed sooner and treated accordingly. These are some of the best and most common diagnosis tests for detecting breast cancer:
Breast examination – This is a physical examination of the breasts that lets the doctor check the breast tissue for lumps. The doctor will check the breasts and the lymph nodes in the armpit for abnormalities.
Mammogram –
This is an x-ray imaging test for the breasts. These are very useful in seeing any abnormal growth in the breast tissue.
Breast ultrasound – Ultrasound test uses high-frequency sound waves to produce detailed of the internal structure within the breast. This test will effectively highlight any type of abnormal lump or mass in the breast.
Biopsy – The surgeon will use minimally invasive surgical method to remove a small portion of the suspected cancerous tissue from within the breast. This breast tissue sample is then sent to a pathology laboratory for detailed analysis.
Breast MRI – The breast magnetic resonance imaging (MRI) is an advanced diagnostic imaging test. It uses powerful magnets and radio waves to create a significantly detailed cross-sectional image of the breast tissue. A contrast dye is often injected before the breast MRI to help highlight any abnormality in the breast tissue.
These tests help in diagnosing breast cancer. If breast cancer is found in a person, then the doctor will advise one of these tests to stage the breast cancer:
- Blood test – A CBC (complete blood count) test is most useful in determining the stage of breast cancer.
- Advanced mammogram
- Breast MRI
- Breast CT (computerized tomography) scan
- Breast PET (positron emission tomography) scan
The staging process helps the doctor to determine the extent of growth of the breast cancer and this in turn helps to determine the best-suited breast cancer treatment for the particular case.
How is Breast Cancer treated?
There are various different methods for treatment of breast cancer. The type of breast cancer treatment mainly depends on several factors, such as the stage of breast cancer, its size, are of affecting along with the patient’s age, overall heath level, etc which the doctor will consider.
These are the various types of breast cancer treatments:
Surgery
Surgical removal of breast cancer is one of the most common and effective treatment methods. In this, there are sub-types of surgical processes that are performed, including:
- Lumpectomy – This is a selective breast cancer surgery treatment for smaller sized breast tumors. The surgeon will use a wide local excision method to remove the cancerous tissue as well as a small margin from the surrounding healthy tissue as well to prevent chances of the cancer from recurring.
- Mastectomy – This is one of the major surgeries for breast cancers. It involves removing the entire breast tissue, including the lobules, fatty tissue, milk ducts, nipple, areola as well as some portion of the skin.
- Sentinel node biopsy – This surgical treatment of breast cancer is helpful in determining if the cancer has spread to the surrounding lymph nodes. The surgeon will remove a few of the closest-situated lymph nodes near the breast to check for cancerous cells or drainage from the tumor.
- Axillary lymph node dissection – In case the surgeon finds cancer cells in the sentinel lymph nodes the additional lymph nodes near the armpit might also need to be removed surgically.
- Contra lateral prophylactic mastectomy – This surgery involves removing both the breast tissues completely even if the cancer is found to be affecting one of the breasts. This is done to prevent the risk of the cancer recurring in the affected breast and the cancer from spreading to the other healthy breast tissue.
Radiotherapy
Radiotherapy, also known as radiation therapy, is a breast cancer treatment method involving the use of high-energy x-rays (or protons) to target and destroy the cancer cells in the breast tissue. Radiotherapy can be done as an external procedure or the surgeon might use minimally invasive surgical method to insert a small radioactive device into the breast (brachytherapy) for closer access in giving an effective radiation dose to the cancerous breast tissue cells.
This is often used in combination with a surgical breast cancer treatment in case the surgery is not able to remove the entire cancerous tissue.
Chemotherapy
Chemotherapy treatment for breast cancer involves using a combination of specially designed medicinal drugs that are aimed to destroy the cancerous cells in the breast. This treatment method is also used before treating a large sized breast tumor. The medicinal drugs are effective in reducing the size of the large cancerous tumor in the breast which can then be safely removed using surgical methods.
Why choose HealthCare Travel Council Of India for Breast Cancer treatment?
HealthCare Travel Council Of India is the worldwide leading medical tourism company. It is globally renowned for providing the most effective and affordable cancer treatment services for patients who wish to travel abroad for breast cancer treatment. HealthCare Travel Council Of India ensures all-round quality in breast cancer treatment and all other services to give the patient a convenient and cost-effective medical treatment.
What is Cancer Radiation Treatment?
Price :- From $ 3000
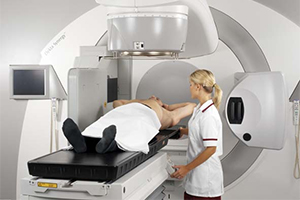
Radiation therapy treatment is a form of therapy for treating cancer treatment that uses x-rays as a means of damaging the DNA of malignant tumor cells. It is also known as “radiotherapy and “radiation oncology”.
Most common types of cancer respond positively to radiation therapy. It is used for many different types of cancers. Radiation therapy will damage normal cells in the process of eradicated cancer cells.
However, most normal cells will recover quickly from the treatment. The main goal of radiotherapy is damage as many cancer cells as possible while minimizing damage to normal cells.
Please refer to the following pages for more information about specific cancer radiation treatments:
- Brain Cancer Radiation Treatment
- Liver Cancer Radiation Treatment
- Lung Cancer Radiation Treatment
- Pancreas Cancer Radiation Treatment
- Spine Cancer Radiation Treatment
Radiation therapy may be used prior to surgery in order to shrink tumors. It can also be used after surgeries to prevent a relapse of cancer cells. Radiation therapy has many applications and may be used either separately or in combination with other types of therapy such as hormone therapy or chemotherapy. For some types of tumors it may be the only type of treatment needed.
How does the Cancer Radiation Treatment Work?
Radiation therapy is generally applied directly to a tumor. For this reason it is considered to be a “localize” therapy. This means that it treats only a specific portion of the body. This is different from “systemic” types of therapies that travel throughout the entire body (such as chemotherapy).
During the procedure, the high energy rays are aimed at the tumor from several different angles. This serves the purpose of avoiding damage to normal cells, while providing a larger dose to the actual tumor. It also helps in allowing the rays to pass through the various layers of tissue and organs without damaging them.
Sometimes the radiation field may encompass small portions of normal tissue or other systems that are involved such as surrounding lymph nodes.
This is because the position of the tumor can sometimes be altered by many factors.
It is important that the entire malignant growth be treated with the rays. These forms of cancer radiation treatment are usually administered once or twice daily
What are the side effects of Cancer Radiation Treatment?
Since radiation therapy inevitably results in damage to healthy cells along with the malignant growths, it can have undesirable side effects.
Depending on the location of the tumor, these may include: alopecia (hair loss), digestive problems, diarrhea, lung damage, urinary problems, changes in sexual function, and other radiation-associated effects.
Recovery time is usually swift, as external beam radiation is usually an outpatient procedure.
Other forms of radiotherapy such as internal radiation therapy may require a few days of hospitalization after the procedure is completed. Side effects can last anywhere from weeks to months. This is considered to be much shorter than other forms of treatment such as chemotherapy.
What is Ovarian Cancer?
Price :- From $ 4000
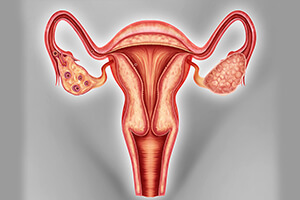
Ovarian cancer is the abnormal growth of tissue cells covering the ovaries. Ovarian cancer originates in the ovaries and can then spread to surrounding parts swiftly. This is one of the more prevalent types of cancer in women and is mostly seen developing in post-menopausal women.
Ovarian cancer can affect cell growth in one or both the ovaries. The ovaries are two small glands on both sides of the uterus. Ovaries produce the female sex hormones, store and release the eggs (ova).
Ovarian cancer can be effectively treated if detected at an early stage.
What are the symptoms of Ovarian Cancer?
In certain cases, ovarian cancer displays early signs, such as:
- Pelvic/abdominal pain
- Frequent bloating
- Eating problems
- Urinary problems – Frequent/urgent urination
The other common symptoms seen for ovarian cancer include:
- Regular indigestion
- Constant fatigue
- Chronic back ache
- Painful intercourse
- Abnormal changes in menstrual cycle
- Frequent constipation
How is Ovarian Cancer diagnosed?
These are the common diagnostic tests and examinations that are helpful in detection, diagnosing and staging of ovarian cancer:
Physical Examination
This includes a pelvic examination and a Pap test. The physical pelvic examination is helpful in finding any abnormal growths (lumps) in the ovaries. The doctor may also advise a recto-vaginal exam to check the internal pelvic organs for cancerous growths.
Biopsy
The doctor will remove a small piece of the suspected ovary through minimally invasive surgical method (laparotomy).The removed sample of the ovary tissue is sent to a pathological laboratory for a detailed analysis.
CA-125
The Cancer Antigen 125 (CA-125) level test is helpful to check for a certain protein which is found over the cancerous ovarian cells.
Pelvic/Trans-vaginal Ultrasound
This ultrasound imaging technique is used to check for abnormal lumps in the ovary.
Imaging diagnostic tests
Other imaging diagnostic tests, such as MRI (Magnetic Resonance Imaging) test and CT (Computerized Tomography) scan are useful for detailed imaging of the internal pelvic region and check for signs of abnormal ovarian growths.
How is Ovarian Cancer treated?
There are several types of treatments for ovarian cancer. The doctor will decide on the most effective ovarian cancer treatment for the individual case depending on various factors, such as age, health status, stage and type of ovarian cancer.
These are the most common ovarian cancer treatment methods that are effective in treating the cancer of the ovaries and also help in preventing it from recurring later on in life:
Chemotherapy
Chemotherapy is the medicinal treatment for ovarian cancer. Chemotherapy is useful in reducing the size of the tumor in the ovaries. This treatment also slows down growth rate of the cancerous cells.
Chemotherapy is mostly advised after a surgical treatment, where the surgeon is not able to remove the cancerous tissue completely using surgical methods alone. Chemotherapy helps to target the blood source of the cancerous cell and shrink its size significantly. This treatment is also advised before a surgical treatment for ovarian cancer to shrink a large-sized ovarian tumor so that it can be safely removed afterwards using surgical methods.
Chemotherapy medications can be administered using:
- Oral method (through the mouth)
- IV (Intravenous) method (through a tube connected to a vein)
- IP (Intra-peritoneal) method (through a thin tube inserted in the body)
Surgical
Surgical treatment is considered to be the main treatment method for ovarian cancer.
There are several surgical procedures that are performed (individually/combined) that are helpful in treating ovarian cancer effectively, such as:
- Total Hysterectomy – This surgical procedure is used to remove the cancer-affected cervix and the uterus.
- Unilateral Salpingo-Oopherectomy – This surgical procedure is used to remove one ovary and fallopian tube that have been affected.
- Bilateral Salpingo-Oopherectomy – This surgical procedure is used to remove both the ovaries and fallopian tubes.
- Omentectomy – This surgical treatment is used to remove the omentum (fatty tissue attached to abdominal organs) when the cancer spreads to other abdominal organs.
Radiotherapy
Radiation therapy for treating ovarian cancer involves targeting the cancerous ovarian cells with high-energy radiation. These particle waves are able to disrupt the cancer growth fast and destroy the cancerous cells within the ovaries.
Why choose HealthCare Travel Council Of India for treatment of Ovarian Cancer?
HealthCare Travel Council Of India is the prime provider of world-class medical tourism all over the globe. HEALTHCARE TRAVEL COUNCIL OF INDIA has association with a wide network of high-standard hospitals and healthcare facilities across the globe that specializes in women’s health and cancer. HEALTHCARE TRAVEL COUNCIL OF INDIA provides all-round assistance for patients to travel abroad to various international destinations, such as Thailand, India, Malaysia, US, UK, etc for effective ovarian cancer treatment at affordable cost.
What is Cervical Cancer?
Price :- From $ 500000

Cervical cancer causes abnormal development in the tissue cells of the cervix. Prompt detection and fast treatment is vital to successfully treat this cancer and prevent additional serous health complications from arising.
What causes Cervical Cancer?
Cervical cancer develops due to the action of the HPV (human papillomavirus). This virus is contacted as an STD (sexually transmitted disease) through unsafe sexual intercourse with an infected person.
Although there are various types of HPV, not all of them result in cervical cancer. Mostly adults are affected with this virus and at times the infection is mild enough to go away on their own. However it is liable to result in serious genital warts that can develop into cervical cancer.
What are the symptoms of Cervical Cancer?
The abnormal changes occurring in the cervical cells when result in development of cervical cancer it causes various symptoms, such as:
- Abnormal vaginal bleeding
- Painful sexual intercourse
- Abnormal vaginal discharge
- Abnormal changes in menstrual cycle
- Anemia (from abnormal vaginal bleeding)
- Constant leg, back or pelvic pain
- Urinary disorders caused by blockage of kidney or ureter
- Leakage of urine/stool into vagina
- Unexplained weight loss
How is Cervical Cancer diagnosed?
There are several diagnostic exams and tests that help detect cervical cancer. An early detection method is used to identify potential cervical cancer, with:
Pap test – This is an early detection technique for cervical cancer. This test is useful in finding abnormal changes in cervical cells, which helps to determine the risk of cervical cancer.
The doctor will take into consideration your age, overall health, weight, etc to schedule the Pap test.
When the doctor suspects cervical cancer, these are the various diagnostic tests that help to confirm the diagnosis:
Cervical Biopsy (Colposcopy) – This test is useful to find if cancer cells have affected the surface of the cervix and the spread of the cancerous cells in it.
Endo-cervical Biopsy (Curettage) – This diagnostic test help to determine if the cancer cells have affected the cervical canal passage.
Cone Biopsy (LEEP – Loop Electrosurgical Excision Procedure) – These series of advanced diagnostic tests help to remove affected cervical tissue for detailed pathological analysis.
The doctor will also recommend several diagnostic tests that help to determine the stage (level of severity) of the cervical cancer, which helps to select the best-suited cervical cancer treatment.
These are the staging tests for cervical cancer:
Chest X-ray Test – This test helps to check lungs for cancer signs.
CT (Computerized Tomography) Scan – A CT Scan helps to use advanced x-ray imaging technique for better viewing of the various organs inside the body for signs of advanced cervical cancer.
Ultrasound Test – This test uses reflecting sound waves to determine abnormalities in the internal organs and soft tissue.
MRI (Magnetic Resonance Imaging) Test – This is a high-tech imaging technique that uses powerful electromagnetic waves to see inside the body with non-invasive diagnostic technique.
How is Cervical Cancer treated?
Cervical cancer detected in the early developmental stages can be successfully treated. There are several factors (such as your age, health status, etc) that will help the doctor determine the best-suited cervical cancer treatment for you.
These are the most common cervical cancer treatment methods:
Chemotherapy
This is the medicinal treatment technique for early-stage and mild form of cervical cancer. This technique uses specially-designed medicinal drugs to combat the abnormally growing cervical cells.
Chemotherapy aims to reduce the size of the cervical tumor by cutting off its blood supply mainly.
Radiotherapy
Radiation therapy is useful for treating specific stages of cervical cancer. This treatment technique is also often used in combination with surgical treatment methods for added effectiveness.
Radiotherapy uses precisely controlled and accurate dosage of high-energy radiation particles (such as x-rays) to target and destroy the cancerous cells from developing. In case the cervical tumor is considerably larger in size then radiotherapy helps to decrease its size which can then be removed using surgical methods.
Surgery
The doctor will advise surgical treatment of cervical cancer depending on the location and extent of cervical cancer as well as future plans for getting pregnant.
Surgical treatment for cervical cancer may include:
- LEEP – This is an innovative surgical treatment that helps to remove a wedge of the cancer-affected cervical tissue.
- Radical Trachelectomy – This surgical technique is used to remove the cervix along with a portion of the vagina and the pelvic lymph nodes as well. The uterus is not removed in this.
- Hysterectomy – This is an extensive surgical treatment for cervical cancer. It removes the cervix and the uterus as well. The doctor may choose to remove the fallopian tubes and ovaries too to prevent the cancer from returning.
- Bilateral Salpingo-Oopherectomy – This surgical treatment for cervical cancer removes the fallopian tubes and both the ovaries.
- Pelvic Exenteration – This is the most extensive pelvic surgical procedure. This surgical treatment for cervical cancer is advised when the cancer has spread to affect the lower abdomen and the pelvic region. This surgery requires removing the bladder, rectum, lower colon, ovaries, vagina, uterus and cervix. Artificial orifices are made to pass out waste from the body efficiently.
Why choose HealthCare Travel Council Of India for Cervical Cancer treatment?
HealthCare Travel Council Of India is the world’s leading popular medical tourism company. HEALTHCARE TRAVEL COUNCIL OF INDIA connects patients with the most renowned cancer specialists to ensure the best diagnosis and treatment for every cervical cancer patient. HEALTHCARE TRAVEL COUNCIL OF INDIA aims to provide global-class medical tourism services at affordable rates to international patients from all over the world.
What is Cancer Treatment?
Price :- From $ After Evaluation

Cancer treatment is a number of conventional and non-conventional medical treatment methods that are used to treat the large varieties of cancers that develop in a person. Cancer treatment varies according to the type of cancer, it’s location, size, physiology, etc.
What are the different kinds of Cancer?
There are different types of cancers that affect people. The cancers are classified mainly according to the specific part of the body which they affect, as well as the types of cancerous cells that are seen in the abnormal tissue growth (or tumor).
Here are the several kinds of cancers:
Carcinoma – Carcinoma affect the epithelial cells in the body. The epithelial cells make up the tissue covering over organs and blood vessels. Carcinoma mostly affects adults. These may be seen in the form of breast cancer, lung cancer, pancreatic cancer, etc.
Sarcoma – Sarcoma affect the connective tissues in the body. Sarcoma affects bones, cartilage and other soft tissues in the body. These are seen as abnormal growth of the mesenchymal cells surrounding the bone marrow.
Lymphoma/Leukemia – Leukemia and lymphoma are the effects of abnormalities in the blood cells. These are known to affect children and adults alike.
Germ Cell Tumor – Germ cell tumor is a cancer that affects the pluripotent cells. Pluripotent cells are the basic cells that later develop into the various types of other cells in the body. This cancer is mostly seen as testicular cancer or ovarian cancer.
Blastoma – Blastoma affect the developing tissues in the embryo. These result in various other complications after birth of the child and are seen in small children.
What are the types of Cancer?
Cancers are categorized according to the part of the body that they affect initially. Below are some of the more common types of cancers that can be seen today:
Brain cancer – Brain cancers are also sub-categorized into several types. Some of the most common brain cancers are cerebellar astrocytoma, ependymoma, malignant glioma, medulloblastoma, etc.
Breast cancer – Breast cancer affects the soft tissue in the breast of women, mainly. Breast cancer is seen in the form of a small abnormal bump or dimple in the breast. It can also be noticed when the size of the breast changes or if there is fluid leakage or a reddish patch on the breast skin.
Cervical cancer – Cervical cancer develops in the cervical region initially, however, it can easily spread to surrounding area. Cervical cancer is mostly detected through constant pelvic pain, painful sexual intercourse and vaginal bleeding among other signs.
Esophageal cancer – Esophageal cancer is also known as throat cancer. This affects the esophagus (food pipe) which connects the mouth to the stomach. Esophageal cancer is often detected when the patient experienced sudden weight loss, trouble in swallowing, change in voice, dry cough, blood in vomit, etc.
Oral cancer – Oral cancer is also known as mouth cancer. It affects the oral cavity (mouth). Oral cancer is seen developing as a lesion in the mouth and quickly spreads to other surrounding tissues.
What are the different types of Cancer Treatments?
As cancer is caused by varying factors and can affect any part of the body, the treatment for cancer also includes several different treatment methods that are proven to be suitable for treating the particular type of cancer.
These are the common conventional and alternate cancer treatment methods:
Surgery
Surgical treatment of cancer is aimed to remove the cancerous tissue (tumor) completely, whenever possible. The surgeon will also remove a marginal portion of the surrounding healthy tissue around the cancerous cells to prevent the risk of the cancer recurring in the future. Surgical methods are used to diagnose and treat cancers.
Radiotherapy
This innovative cancer treatment method involves using high-energy radiation beams to destroy cancerous cells. Radiation therapy uses ionizing radiation technology to destroy suspected and confirmed cancer cells from almost any part of the body.
Radiations therapy can be administered from outside the body, which is the conventional form. A new and innovative radiation therapy for cancer treatment involves inserting a small radioactive device into the body and focusing radiation on to the cancerous cells from the nearest possible location. This is a more precise and accurate form of radiotherapy as it decreases the risk of damage to surrounding healthy tissue from the radiation beams.
Chemotherapy
Chemotherapy is a medical cancer treatment. Chemotherapy involves using a combination of advanced medicinal drugs that are designed to destroy cancer cells.
Chemotherapy is also useful as a preventive measure to stop the growth (spread) of the cancerous cells to affect surrounding healthy tissue.
Immunotherapy
Immunotherapy requires the oncologist to use a variety of innovative techniques that stimulate the patient’s immune system. This technique enables the natural immune system to get the strength to destroy the cancer cells in the body.
Why choose HealthCare Travel Council Of India for Cancer Treatment?
HealthCare Travel Council Of India is especially known to provide extensive cancer treatment services. HEALTHCARE TRAVEL COUNCIL OF INDIA is connected to the largest global network of world-class cancer specialty hospitals. These reliable and efficient cancer care hospitals are located in popular international destinations, such as India, US, UK, Thailand, Dubai, etc for better convenience to patients travelling abroad for cancer treatment. HEALTHCARE TRAVEL COUNCIL OF INDIA is committed to providing assistance to patients for getting the best, most effective and affordable cancer treatment.
Andrology & Urology – An Overview
Price:- From ₹ After Evaluation
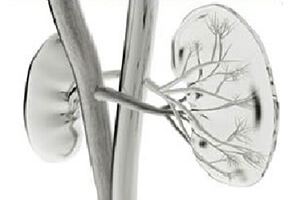
Andrology and Urology and two streams of medicine and surgery that treat the variety of disorders, diseases or damage that the male and female urinary tract may suffer. Andrology and Urology combine to treat medical problems relating to adrenal glands, bladder, kidney, testis, prostate gland, urethra and penis.
What are the various Andrology and Urology disorders?
These are some of the most commonly treated medical disorders and conditions in Andrology and Urology:
Cancer/Benign tumors
Andrology and urology often require treatment of a large variety of tumors that affect any part of the male urinary system. The treatments in this section include medical and surgical treatment for renal cancer, adrenal cancer, ureteral cancer, renal pelvic cancer, bladder cancer, prostate cancer, penile cancer, testicular cancer, etc.
Urolithiasis
Also known as ‘kidney stones’ more commonly, this condition is effectively treated by various medicinal drugs, or in emergency or aggravated conditions, the doctor/physician may advise on a surgical options for its treatment.
Voiding difficulty
These are some of the urinary inconsistency problems that are seen mostly in women. These are mostly known to be caused by neurogenic bladder, interstitial cystitis and an overactive bladder.
Male infertility
There are various conditions relevant to causing male infertility, such as erectile dysfunction a variety of other medical disorders. The treatment options vary according to the type of disorder as well as its severity.
Chronic kidney disease
There are a large range of medical disorders that can develop into serious problems with the renal (kidney) functions. These are mainly treated with advanced medical treatment techniques, such as hemodialysis, peritoneal dialysis and kidney (renal) transplant.
Congenital urological disorders
These are a range of birth-defects that are seen affecting a person’s urinary system. In men, these are mostly seen in the form of undescended testis and ureteropelvic cystitis. There are a variety of surgical options useful for treating these and similar other conditions effectively.
Infections
There are various types of infections that can develop in the male urinary tract, such as prostalitis, cystitis and epididymitis. These often result in painful and constant uncomfortable conditions in the patient. There are medical and surgical treatments for these infections.
What are the various Andrology and Urology treatments?
Today, with the huge progress made in medical and surgical technology, there are various innovative and highly-effective Andrology and Urology treatments available to treat the large numbers of medical diseases, disorders or trauma that affect person’s urinary tract.
Let us look at some of the most advanced Andrology and Urology treatment methods:
Robotic Laparoscopic Radical Prostatectomy
This is a highly-advanced and safer prostatectomy procedure. It requires the surgeon using high-tech robotic surgical system to remove the damaged prostate with minimal surgical invasion in the body.
Laparoscopic Adrenalectomy/Nephrectomy
This is also an advanced minimally invasive surgical method that uses special surgical instruments to remove the adrenal gland or the prostate gland when they are damaged or malfunctioning.
Minimally Invasive Endoscopic Surgery
This is actually an umbrella term used to describe a number of innovative least-invasive surgical techniques that are being increasingly used, not only in Andrology and Urology surgical treatments but also in treating a large number of other medical disorders as well.
Bladder Hydro distention
This is an effective diagnostic technique. Bladder hydro distention requires the surgeon to fill the bladder with a saline water solution. This allows the doctor to check for ‘glomerulations’, which are small points that bleed once injected water solution puts sufficient pressure in the bladder when the patient is suffering from interstitial cystitis.
Brachytherapy
This is an advanced cancer treatment technique. It requires the surgeon to insert a small radioactive source near to the cancer/tumor and then bombard it with radiation from a closer range than an outer conventional radiotherapy treatment of cancer can. This is a comparatively safer radiotherapy method as it prevents the surrounding healthy tissue to be damaged from the radiation being used to destroy the cancerous cells.
Uroflowmetry
This is a minimally invasive diagnostic technique. It requires the doctor to measure the consistency of the flow of urine in a person. This is a common diagnostic test to determine the source of pain felt during urination or for the inconsistencies in urination process.
Renal biopsy
A renal biopsy is basically a minimally invasive surgical diagnostic technique where the surgeon will remove a small portion of the damaged kidney. This removed portion is meant to be sent to a pathological laboratory for better and detailed analysis.
HealthCare Travel Council Of India always aims to provide each patient with the best-in-class Andrology and Urology treatments in India, as well as other major international destinations all over the world. Thousands of patients suffering from a large variety of urological disorders have received effective treatment for their ailments. HealthCare Travel Council Of India ensures that each patient gets connected with the most experienced Andrology and Urology specialist to get the ideal and successful treatment for their problems. HealthCare Travel Council Of India is popular for providing the most convenient and cost-effective customized tourism assistance for getting medical treatments all over the world.
What are the various Obstetric and Gynecological disorders and their treatments?
Price:- From ₹ After Evaluation

An obstetric-gynecologists work entails treating vast number of medical disorders that affect a woman’s reproductive system mainly. The complete list of medical problems treated through OB-GYN expertise is extensive sub-categorized and classified into various segments.
Some of the most common obstetric and gynecological disorders and their effective treatments are:
Female Pelvic Medicine/Reconstructive Surgery
These medical disorders/injuries are mainly in the pelvic region in women. Although, there are various disorders and treatments for such disorders, the most commonly seen are:
- Pelvic organ collapse – This causes pelvic organs to lose their place and form hernias. Pelvic organs, such as uterus, apex/posterior vaginal structure, etc which can experience varying degrees of prolapse, especially due to advancing age.
- Vesicovaginal fistula (VVF) – VVF is another form of UGF (uro-genital fistula) which forms a fistulous path from the bladder to the vagina. This results in constant involuntary discharge of urine into the vault of the vagina.
General Gynecology
This segment of OB-GYN handles a large variety of medical disorders that are commonly seen affecting the reproductive system, as well as general women’s well-being.
These are some of the most commonly treated general gynecological disorders:
- Menorrhagia – Heavy menstrual periods which are not normal are treated using various methods.
- Metrorrhagia – Another menstrual condition that causes irregular menstrual periods.
- Ovarian cysts – Small abnormal growth seen developing in the walls of the ovaries, which at times can create more uncomfortable and painful complications.
Minimally Invasive Gynecology Surgery
This is one of the most advanced and effective form of surgical procedure that is used in various forms to perform the best and most efficient surgical treatment for a variety of gynecological disorders.
Some of the most advanced minimally invasive gynecological treatment techniques include:
- Cervical Loop Electrode Excision Procedure (LEEP)
- Diagnostic hysteroscopy
- Diagnostic laparoscopy
- CO2 Laser treatment
- Endometrial ablation
- Operative hysteroscopy – (to remove polyps, fibroids, uterine septa and sterilization)
- Operative laparoscopy – (to remove fallopian tubes, ovaries, ovarian cysts and for sterilization, etc)
- Vulvar vestibulectomy
Gynecological Oncology
Another important part of the OB-GYN field is the detection, diagnosis, treatment, palliative care and other services for the large variety of cancers (malignant and benign) that affect a woman’s reproductive system, such as:
- Ovarian cancer
- Vaginal cancer
- Vulva cancer
The treatments for these cancers mostly include a number of effective treatment methods, such as chemotherapy, radiotherapy or surgery. Hysterectomies may be advised by doctors in case it can easily treat non-cancerous conditions.
HealthCare Travel Council Of India has been providing effective and convenient obstetric and gynecological healthcare treatment to thousands of women across the world. HEALTHCARE TRAVEL COUNCIL OF INDIA is renowned world-wide for providing fast communication between patient and OB-GYN experts. HealthCare Travel Council Of India offers medical treatments in various popular international destinations, including India, US, UK, Thailand and Dubai according to the patient’s convenience.
What is Brain Tumor?
Price:- From ₹ After Evaluation
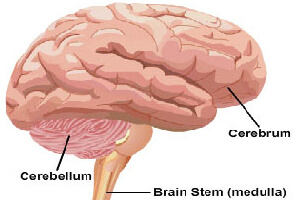
A brain tumor is defined as an abnormal growth of cells in the brain tissue. These are categorized into two kinds:
Benign Brain Tumors
A benign brain tumor is non-cancerous, in the sense that it is not at risk of spreading. Benign brain tumors are clearly defined and are mostly superficial on the brain. This makes it easier to remove them surgically if they are in a part of the brain which is efficiently accessible.
Malignant Brain Tumors
Malignant brain tumors are primary brain tumors which also originate in the brain and grow faster than a benign brain tumor. These are cancerous in nature that grow and spread to affect the surrounding healthy tissue as well. These are known to spread to other parts of the brain and the central nervous system as well.
Malignant brain tissues grow larger in size as well as spread more widely to affect the surrounding healthy tissue. The brain tissue gets inflamed and experiences increasing pressure due to the growing cells and the skull.
How can you identify the signs and symptoms of Brain Tumor?
The signs and symptoms of brain tumor varies according to the type, size and its location in the brain. The location of the brain tumor will mostly decide the symptoms, as small areas of the brain are designed to control varying body functions.
Some of the brain tumors may be benign and not show any noticeable signs until they are considerably larger in size and then immediately cause a series of dangerous effects on the body. At the same times, most brain tumors are slow in growth and show various signs and symptoms as they develop.
The most common problem seen in brain tumor cases is the constant headaches. These frequent and randomly occurring headaches are usually not treated with conventional medicinal treatment. However, such headaches may also be experienced due to other reasons than a brain tumor as well.
Most of the commonly seen symptoms of brain tumors are:
• Seizures
• Damaged vision
• Damaged speech
• Damaged hearing
• Balancing problem
• Walking problem
• Tingling/numbness in arm or leg
• Memory problems
• Changes in personality
• Concentration problems
• Weakness in a specific part of the body
Although these symptoms can also be caused due to a variety of other reasons, it is always advisable to seek quick medical consultation in case any of these symptoms are seen.
How are Brain Tumors diagnosed?
The physician or doctor usually begin investigation into a suspected brain tumor case by asking familiar questions, such as previous medical history, prevalence of brain tumor in the family, complete physical exam as well as a series of advanced diagnostic tests to confirm.
One of the following tests is usually performed to determine the presence of brain tumor in a person:
Imaging tests
The doctor may advise to undergo CT (computerized tomography) scan or an MRI (magnetic resonance imaging) tests to get a good look at the suspected brain tumor.
Angiogram/MRA – This involves using a minimally invasive surgical method. The procedure requires first injecting an organic dye and use advanced x-ray imaging technology to view the blood vessels in the brain and look for abnormalities in the blood supply indicating towards an anomaly.
Another method for determining the presence and the type of brain tumor is biopsy. This requires making an incision to reach the suspected tumor mass in the brain. Today, with advanced surgical technology doctors can perform this procedure on a patient using least invasive surgical methods that require a very short time and are also considerably safer. The biopsy procedure requires the doctor to remove a small portion of the abnormal tissue and analyze it in detail at a pathology laboratory.
How are Brain Tumors treated?
There are a variety of conventional and innovative treatment methods for brain tumors. The doctor will consider various factors, such as the type, size and location of the tumor as well as your overall health to decide the best-suited and most effective brain tumor treatment method.
These are the various brain tumor treatment methods:
Surgery
Surgical removal of brain tumor is one of the most common methods of brain tumor treatment. The surgeon will usually remove the entire tumor as well as a small part of the surrounding healthy tissue to prevent the risk of the cancer recurring in the future.
Surgery is usually one of the priority treatments for brain tumors, if the tumor is situated in a part of the brain which is easily accessible to a surgeon and there is no risk of damage to the surrounding healthy tissue and parts of the brain.
In case the tumor is in a considerably inaccessible part of the brain, the surgeon will then remove much of the tumor mass with surgical methods and the remaining part of the tumor is eventually destroyed with another tumor treatment technique, such as chemotherapy or radiotherapy.
Radiotherapy
Radiation therapy (or radiotherapy) is another non-invasive brain tumor treatment technique. This uses high-energy x-rays (or similar particle waves) to destroy cancerous tumor cells. This treatment method is also useful in slowing the growth as well as stopping the growth of the brain tumor completely.
Chemotherapy
This brain tumor treatment method requires using a variety of strong medicinal drugs to target and destroy the tumor cells. These drugs are designed to attack the tumor cells’ ability to divide and grow. This method is mostly used in combination with another brain tumor treatment method, such as surgery or radiotherapy, for most effective treatment.
HealthCare Travel Council Of India provides the best in effective and convenient brain tumor treatment. The company is known for providing efficient healthcare and cancer treatment in more than six popular global destinations, including US, UK and India. Effective connection for patients to expert healthcare professionals and providing comprehensive travel packages for patients to travel for a variety of medical and surgical treatments is the main function of HealthCare Travel Council Of India.